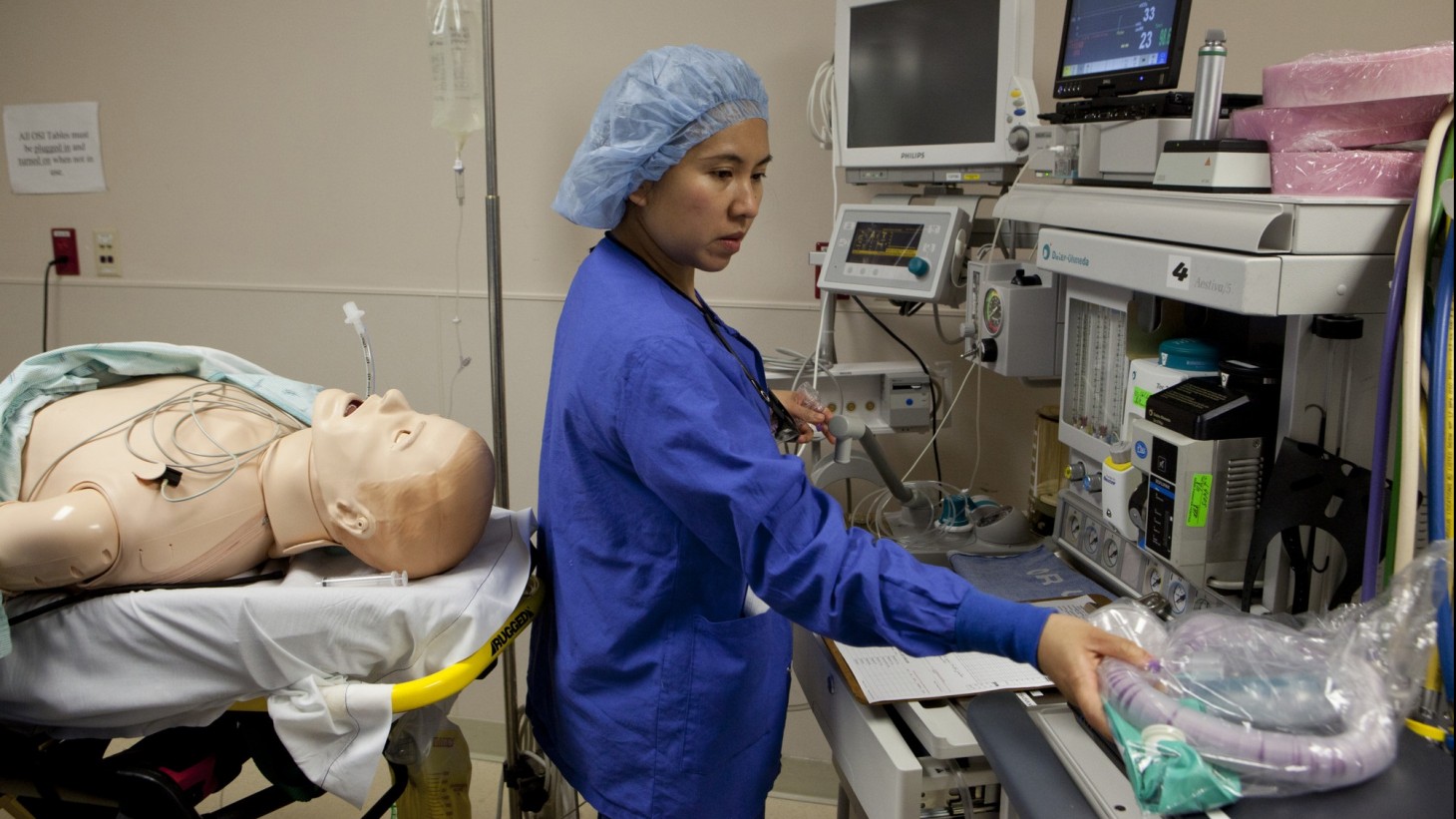
Fake patient, real issues: Unit-based teams, like this anasthesia department at the Sunnyside Hospital in the Northwest region, have used simulations to explore better ways of keeping patients safe during surgery.
Unit-based teams have huge potential for improving patient safety. So why are so few taking it on?
The patient in the operating room was moaning and suffering sudden seizures. A half-dozen caregivers crowded around him, attempting to stabilize him as they watched his vital signs on a monitor.
This might have been a normal June afternoon in the OR at Sunnyside Medical Center in the Northwest region—except the patient was a mannequin. The staff members were being videotaped as part of a simulation to help operating room personnel learn and practice effective techniques for keeping patients safe during and after surgeries. Afterward, they did a debrief, discussing what worked and what didn’t with their unusual patient.
It’s all part of how this regional surgical services team, composed of the co-leads of several unit-based teams at different ambulatory care centers and at Sunnyside, operates. From 2009 to 2010, for example, it reduced the rate of surgical site infections by an impressive 32 percent. These results came from implementing proven practices for reducing infections, such as safety simulations, hand hygiene and clipping (rather than shaving) patients’ hair at the surgical site.
They also came from an explicit effort to change the culture standing in the way of patient safety. A 2010 safety summit involved everyone in the associated departments—from surgeons to techs to EVS workers, inpatient and ambulatory. Team members shared best practices and discussed ways to have an open dialogue so that when something isn’t right, each person has the accountability and the freedom to speak up.
“In the past,” says surgeon Waleed Lutfiyya, “everyone had a single role and couldn’t break out of that role. There were defined borders about what someone could say. That can create obstacles.”
Now, he says, “The idea is that by working together as a team, everyone has an equal role with the patient. Everyone is equally important.”
The summit included a presentation on the importance of developing a culture of safety.
“Team behaviors do matter,” says Lutfiyya. “Team behaviors affect clinical outcomes.”
Research backs him up. A 2009 study published in The American Journal of Surgery tracked nearly 300 observations by RNs of operations at four Kaiser Permanente sites. The conclusion: Patients whose surgical teams exhibited fewer teamwork behaviors were at a higher risk for death or complications. These observable behaviors revolved around information sharing during various phases of surgery.
In short: Patient safety depends on good communication. From there, it’s easy to see that, since unit-based teams provide a structure and the tools for improving team communication, they are a path to improving patient safety.
Perfectly logical, right? Yet only a tiny fraction of UBT projects aim to improve patient safety, according to data in UBT Tracker, the programwide system for reporting on unit-based teams.
What’s going on? Patient safety projects seem like ideal candidates for unit-based teams, touching all four points of the Value Compass. Keeping patients safe from harm delivers on best quality and best service. Such projects address affordability: In the Northwest, the decrease in infections for the specific procedures being monitored has resulted in an estimated cost avoidance of $220,000. Patient injuries can be devastating to individual and team morale, so intentional efforts to minimize them help create the best place to work.
And who benefits or suffers most if teams do or don’t take on this work?
“We all owe it to the patient,” says Doug Bonacum, Kaiser Permanente’s vice president of Safety Management. “We need to find ways to help people reach deep down and say, ‘I am not comfortable, I have a safety concern.’ It is top down and bottom up. It has to be both.”
When top-down transforms into teamwork
The fact is, there is plenty of work going on throughout Kaiser Permanente on patient safety. Much of it, however, has a top-down, mandatory quality to it—with little or no emphasis on involving frontline staff on how to go about meeting the goals and improving performance.
In the Northwest, for example, switching to a new dress code based on Association of periOperative Registered Nurses (AORN) recommendations was a top-down mandate. One of the changes included replacing the skull cap, which did not always cover all of a person’s hair, with a bouffant cap.
“We assumed, ‘Well, this is the right thing to do for the patient,’ and staff would just do it,” says Claire Spanbock, the regional ambulatory surgery director, acknowledging the limits of the approach. But, “We had people we had to tell again and again. We realized we were making a big change and not involving them….We got there, but it was tough.”
In contrast, when it came to hand hygiene, members of the regional OR UBT sat down together and revised the audit tool several times before settling on the best version.
“You are never going to do this until you have the hearts and minds of the staff,” says Spanbock.
When the right eye is the wrong eye
One reason relatively few teams are working on patient safety may be that until a team has strong communication skills in place—developed in the course of working on simpler improvement projects—its members may shy away from high-stakes efforts.
The Northeast Ohio ophthalmology team already was one of the highest-performing UBTs in the Ohio region when it decided to not take the team’s clean safety record for granted. Its co-leads—the ophthalmologist, ophthalmic technicians and manager—worked together to implement a patient safety briefing immediately prior to all eye procedures.
The idea is an enhanced version of a timeout, when a surgery team pauses before a procedure to engage in a structured communication with the patient to verify key information. It came from the ambulatory surgery center at the Parma Medical Center, where several ophthalmology staff members work.
“We just felt that it would be wise to be proactive,” says Ralph Stewart, MD, the team’s physician co-lead. “There’s no danger of cutting off a leg in our department, but you do need to think about right eye or left eye.”
The team already had worked together to improve wait times and courtesy and helpfulness of staff, so had built the trust and free-flowing communication culture that is at the heart of patient safety efforts. It embraced the idea and, after resolving concerns about the time the safety briefing would take, began brainstorming about what the ophthalmology timeout would be like.
“We split into two different groups that included physicians and technicians, and we discussed which part was going to be the responsibility of the ophthalmologist and which was going to be the responsibility of the technician,” says Renee Paris, a lead ophthalmic technician and an OPEIU Local 17 member.
“It took us a couple of months to get it together,” says Bonna Gochenour, an RN and the team’s management co-lead. “We had to create some ‘smart phrases’ to help us with documentation. When the technician goes into the room with the patient, they’re going to confirm with the patient which eye it is, and the tech puts a little smiley face over the correct eye.” The doctor then does a second verification before beginning the procedure.
In late January, in a textbook small test of change, the team piloted the safety briefing for one month with one physician and one tech.
After a few adjustments—like making sure each procedure room has its own supply of the stickers—the UBT implemented the procedure throughout the department, which encompasses teams at four different facilities in three counties.
Sandy Cireddu, a certified ophthalmic technician and the team’s labor co-lead, is proud of the accomplishments. She thinks the open channel of communication developed through the UBT has been critical to its success.
“Everybody needs to be heard,” says Cireddu, a member of OPEIU Local 17, “and everyone needs to feel you’re on equal ground when you’re discussing these things, so that you can get buy-in.”
Surgical site infections down
At the Woodland Hills Medical Center in Southern California, a campaign to reduce surgical site infections in the labor and delivery department is working.
The department dropped from a rate of five surgical site infections per 100 caesarean sections performed in the second quarter of 2009 to none in the second quarter of 2010.
After a brief rise, the rate headed down again; at the end of the first quarter of 2011, it was less than one per 100. Moreover, the only infections since the third quarter of 2009 have been superficial; there have been no deep or organ-space infections.
The campaign includes a focus on pre-op skin prep, educating new moms on post-op wound care, prophylactic antibiotics, hand hygiene, and trying to reduce traffic flow of staff and families near the operating rooms.
And, as in the Northwest, the effort included enforcement of the AORN guidelines for surgical attire. Out went the skull caps sewn by Min Tan, an obstetrics tech and SEIU UHW member, who helped her colleagues spice up their scrubs by making them custom caps with their favorite patterns—anything ranging from the L.A. Lakers basketball team to spicy-colored chili peppers.
She took the new dress code in stride. “The Labor Management Partnership is about fixing things,” says Tan. “It helps us in not finger-pointing and blaming. It’s not as intimidating as ‘the old days.’ ”
The department’s labor co-lead, Robin Roby, an RN and UNAC/UHCP member, agrees.
“We are becoming part of the solution,” she says. “You feel like you are more involved with what goes on in the unit.”
That involvement is what makes UBTs a foundation for improving patient safety; engagement is the key to effective implementation.
Louise Matheus, the department administrator at Woodland Hills’ labor and delivery unit, acknowledges that focusing on reducing infections was a management decision. But, she says, the department’s progress in controlling infections “is a UBT effort because we involved the whole staff” in implementing the changes.
And Matheus makes it clear she’s looking forward to the day when frontline physicians, managers, nurses and techs use the leverage created by unit-based teams to accelerate improvements in patient safety.
When that day comes, she says, “It won’t be small test of change—it will be large test of change.”
